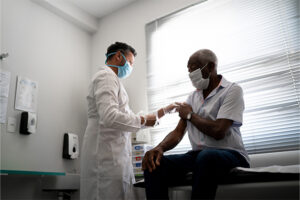
Infectious Diseases
Adult Vaccinations
The Role of the Physician-Patient Relationship in Improving Adult Vaccination Rates for Underserved Communities
This article for developing awareness surrounding racial and ethnic disparities in care was funded by GSK.
Dr Karen Krueger is contracted by GSK and is compensated for the development of this article.
Adult vaccination rates lag behind public health preventative care benchmarks across many common diseases. Healthcare providers have the ability to encourage their adult patients to receive appropriate preventative vaccinations, but they must be informed and responsive to the barriers to care that many patients face. Using tools to build trusting communication between patient and provider is one piece of the puzzle.
Adult vaccination rates for common and preventable diseases, such as pneumococcal pneumonia, influenza, herpes zoster, and human papilloma virus are below public health preventative care benchmarks, and this trend is especially pronounced in our most underserved communities, including African American and Latinx people. Although some barriers these patients face may be beyond the control of any individual doctor, there is one that providers can take immediate action to address: the patient-physician relationship. In my clinical practice, I nurture trusting relationships with patients using strategies grounded in an understanding of common obstacles such relationships face.
For example, in one study of genetic counseling for breast cancer risks, black women reported that they often feel “talked about” instead of “talked to” by their physician or other healthcare professional. This impedes their ability to participate in joint decision-making, which can lead to a disconnect between what the physician thinks the patient should do and what the material reality of the patient’s life can support. And while physicians may view themselves as the most important and trustworthy source of medical information, many Latinx people see self-management, friends and family, and traditional remedies as primary sources of such guidance. A further barrier to communication can be physician assumptions based on patterns that may hold true for white patients but are not universally applicable. Many Pacific Islander ethnic groups, for example, do not show the same correlation between socioeconomic status and vaccine hesitancy that holds true for other ethnic groups. I find it takes consistent effort to identify and challenge the unconscious assumptions I may carry when talking with a patient. The trainings my institutions offer on this topic are useful, but even more useful is applying their lessons in my day-to-day practice.
The disconnect between patient reality and provider expectation may be illustrated by the lower pneumococcal vaccination rates among people with a greater number of health conditions. While providers may prioritize vaccination because they know pneumococcal disease is more dangerous for these populations, their patients may not have the energy or resources to expend on such preventative measures. Instead of insisting these patients share our priorities, we can help them make informed decisions about their health. If we believe something is critically important, we can make it easier to access, perhaps by combining a vaccine appointment with their next regularly scheduled visit, or coordinating vaccine administration with their pharmacist. I have found that a conversation grounded in such joint decision-making empowers patients to become active partners in managing their health.
At the same time, physicians are dealing with our own competing priorities and may not think to recommend all vaccines a patient may be eligible for and benefit from. This continues to be the case for the HPV vaccine, for example, where vaccination rates are still low in this country despite overwhelming evidence that vaccination can greatly reduce risk of several cancers, including cervical, vulvar, and vaginal cancer in females, and penile cancer in males. The reasons for this are multifactorial, but one reason is that healthcare providers may be missing opportunities to recommend and/or administer the vaccine. Ensuring we discuss all preventative tools available, thereby hopefully lowering patients’ future dependence on the systems they have struggled to access, is one way we can build trust. The use of electronic health records can automate this process and alert us to any recommended vaccines, as well as sending patients reminders so they have the time to schedule such visits into their busy lives.
Using this technology allows my face-to-face appointment time to be spent discussing the patients’ priorities and views on vaccine options. I start any conversation by gauging the patient’s level of interest in a particular vaccine. I also ask them about concerns they may have, including any negative information they may have heard from people they know and trust, as well as traditional and social media sources. I take this information seriously and do not criticize my patient for sharing it, since such judgment would be self-defeating. Once I have listened thoroughly, I share both my clinical perspective and any relevant personal and professional experience I may have, which demonstrates that I am personally invested in our relationship and not simply giving commands. In my experience, such respectful and culturally informed conversations can have a positive impact on my relationships with patients, creating an environment in which we both feel safe to challenge preconceptions and make a treatment plan that is right for each patient.
Almario CV, May FP, Maxwell AE, et al. Persistent racial and ethnic disparities in flu vaccination coverage: Results from a population-based study. Am J Infect Control. 2016;44(9):1004-1009. doi:10.1016/j.ajic.2016.03.064
Austin S, Ramamonjiarivelo Z, Comer-HaGans D, Pisu M. Trends and racial/ethnic disparities in pneumococcal polysaccharide vaccination. Popul Health Manag. 2018;21(6):509-516. doi:10.1089/pop.2017.0176
Harpaz R, Leung J. When zoster hits close to home: Impact of personal zoster awareness on zoster vaccine uptake in the U.S. Vaccine. 2017;35(27):3457-3460. doi:10.1016/j.vaccine.2017.04.072
Henderson V, Chukwudozie IB, Comer-Hagans D, et al. Development of a culturally sensitive narrative intervention to promote genetic counseling among African American women at risk for hereditary breast cancer. Cancer. 2021;127(14):2535-2544. doi:10.1002/cncr.33525
Larkey LK, Hecht ML, Miller K, Alatorre C. Hispanic cultural norms for health-seeking behaviors in the face of symptoms. Health Educ Behav. 2001;28(1):65-80. doi:10.1177/109019810102800107
Peterson CE, Dykens JA, Brewer NT, et al. Society of behavioral medicine supports increasing HPV vaccination uptake: an urgent opportunity for cancer prevention. Transl Behav Med. 2016;6(4):672-675. doi:10.1007/s13142-016-0441-5
Samoa RA, Ðoàn LN, Saw A, Aitaoto N, Takeuchi D. Socioeconomic inequities in vaccine hesitancy among Native Hawaiians and Pacific Islanders. Health Equity. 2022;6(1):616-624. doi:10.1089/heq.2022.0033
Schiffman M, Castle PE. The promise of global cervical-cancer prevention. N Engl J Med. 2005;353(20):2101–2104. doi:10.1056/NEJMp058171
Vaccination coverage among adults in the United States, National Health Interview Survey, 2019-2020. Centers for Disease Control and Prevention. 2023. https://www.cdc.gov/vaccines/imz-managers/coverage/adultvaxview/pubs-resources/vaccination-coverage-adults-2019-2020.html. Accessed September 26, 2023.
Vaccination programs: client reminder and recall systems. Guide to Community Preventive Services. https://www.thecommunityguide.org/findings/vaccination-programs-client-reminder-and-recall-systems.html. Accessed September 20, 2023.
Trademarks are property of their respective owners.
©2023 GSK or licensor.
ABXOGM230003 November 2023