
Latest In Conference Reporter
More in Expert Perspectives

Allergy & Immunology
Validated Tools to Assist in the Assessment and Management of Chronic Spontaneous Urticaria

Allergy & Immunology
Chronic Spontaneous Urticaria in Children and Adults: Presentation, Course, and Management Considerations
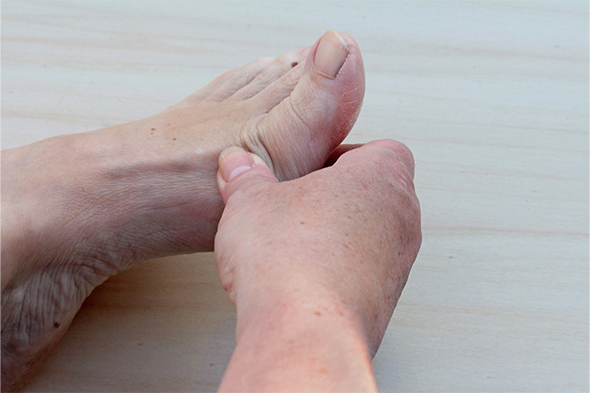
Dermatology
Challenges in the Treatment of Palmoplantar Psoriasis
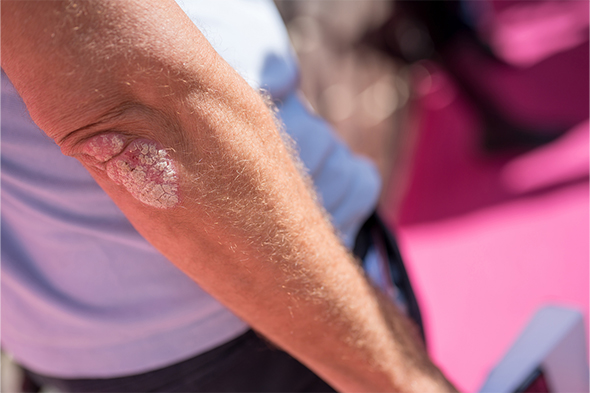
Dermatology
Plaque Psoriasis and the Value of Patient-Identified Treatment Goals
Dermatology
Identifying Biomarkers of Treatment Response in Plaque Psoriasis
Load More















